The Garron Family Cancer Centre
In January 2008, SickKids launched the Comprehensive Cancer Centre. The Centre was designed to enhance and integrate all aspects of clinical, research and educational activities in the discipline of oncology at SickKids.
Two years later, in 2010, the Garron Family donated an unprecedented $30 million to SickKids to revolutionize the care and treatment of children’s cancer in Canada and around the world.
The donation transformed the Comprehensive Cancer Centre into the Garron Family Cancer Centre (GFCC), the largest paediatric oncology centre in Canada, and created five Endowed Chairs in Childhood Cancer Research. A generous new gift of $15 million over 15 years from the Garron family, beginning in 2021, will support the Garron Family Chairs in Childhoood Cancer Research and other high priority needs of the centre.
Translation of new knowledge at the GFCC continues to transform clinical practice and improve clinical outcomes and quality of life for children and their families affected by cancer. Our vision is better outcomes for children with cancer though collaboration, innovation, and discovery.

Meet the Garron Family
Myron and Berna Garron’s son Michael was treated for cancer at SickKids for many years. In 1975, Michael passed away at age 13 from synovial sarcoma, a rare type of soft tissue cancer. Their unprecedented gift is an acknowledgement of the dedication and level of care Michael received and a commitment to help create more positive outcomes for childhood cancer patients and their families.

Centre activities
Discover how we are improving outcomes for children and young adults with cancer through innovative, multidisciplinary research.
View fellowship opportunities and current GFCC Fellows.

We are the largest paediatric Haematoloty/Oncology Program in Canada.
Centre leadership
The GFCC is an innovative and collaborative virtual centre that brings together scientists, clinicians, and educators across multiple disciplines to advance the diagnosis, treatment and outcomes of children, adolescents and young adults with cancer. GFCC faculty is far-reaching and its collaborators can be found throughout numerous divisions, departments and programs within the Hospital, Research Institute and the broader community.
- Linette Margallo, MN
- James Whitlock, MD (Chair)
- Cynthia Hawkins, PhD, MD, FRCPC
- David Brownstone, MSW, RSW
- Jane McGlade, PhD
- Jason Moffat, PhD
- Judy Van Clieaf, RN, BScN, MN
- Marie Bomba, B.Sc., M.Sc., MBA (Ex officio)
- Meredith Irwin, MD
- Paul Nathan, MD, M.Sc., FRCPC
- Peter Dirks, MD, PhD, FRCSC
- Sue Zupanec, NP, MN
- Ulana Bochnewicz, HBA (Ex officio)
- Vijay Ramaswamy, MD
- Kathryn Breckbill, PMP
- Donna Berry, PhD

Garron Family Psychosocial Hematology/Oncology Program
A childhood cancer diagnosis is distressing for the whole family including your child, siblings, caregivers, and other family members. The many changes ahead can be overwhelming, confusing, and can lead to mental-health struggles. To support children and families the Garron Family Psychosocial Hematology/Oncology Program provides critically important psychosocial care and practical resources for patients, families, and caregivers. We are thankful to our generous donors who believe in our shared goals to support children and their families through their cancer journey with the critically important supports and mental-health resources that help improve quality of life. Without their support we could not achieve our goals. Our deepest gratitude to the Garron Family, Kindred Foundation and the Murphy Family Foundation.

KiCS/PROFYLE
In 2016, SickKids established the world-leading SickKids Cancer Sequencing (KiCS) Program, which was designed to analyze the genetic make-up of a child’s cancer to determine a patient’s unique genetic fingerprint, identify the cause of the tumor, gain information about prognosis, and implement personalized treatments. Together with PROFYLE, a trailblazing pan-Canadian program being conducted in partnership with the Terry Fox Research Institute, multiple childhood cancer foundcations, and all 16 paediatric cancer programs across Canada, KiCS matches nationally-collected sequencing data with potentially life-saving drugs.

New Agent and Innovative Therapy (NAIT) program
The New Agent and Innovative Therapy program (NAIT) at SickKids is supported in part by the GFCC and is focused on providing access to new drugs and other treatments for childhood cancer patients. For more information about current clinical trials and eligibility, contact us today.
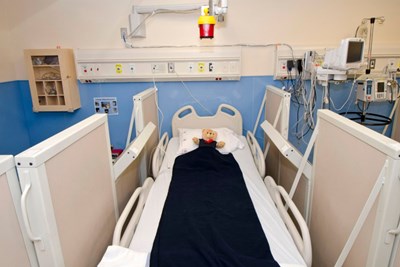
MIBG Program
To deliver this targeted radiation safely to children, and to keep families and hospital staff safe, a specialized room, equipment and healthcare team with special training are needed. SickKids' MIBG room includes state-of-the-art equipment and specialized Neuroblastoma and MIBG Therapy Programs.

Patient referrals for early phase trials
SickKids is a major referral centre across the country for early phase trials conducted by childhood cancer clinical trials consortia such as the Children’s Oncology Group (COG), the National Cancer Institute’s New Approaches to Neuroblastoma Therapy (NANT), the Pacific Pediatric Bone Marrow Transplant Consortium (PBMTC), the Pediatric Neuro-Oncology Consortium (PNOC), Pediatric Brain Tumor Consortium (PBTC), the Pediatric Cancer Immunotherpay Trials Network (PedCITN), and the Collaborative Network for Neuro-Oncology Clinical Trials (CONNECT).
If you are a patient of family member preparing for a visit to SickKids for oncology care, or are a health-care provider looking to refer a patient to SickKids, please refer to the Division of Haematology/Oncology for more information.
A look at CAR T-Cell Therapy at SickKids
Join Marky, a brave patient from SickKids, as we explore the groundbreaking world of CAR T-cell therapy: an innovative, immunotherapy treatment for paediatric cancers like leukemia and lymphoma.

The Blina Backpack
Patients, parents and clinicians collaborated to inform the design for an innovative backpack that delivers an at-home, 28-day continuous infusion of the cancer immunotherapy blinatumomab.

December 7, 2024
Global clinical trial shows improved survival rates for common childhood leukemia
SickKids co-led study shows disease-free survival rates increased to up to 97.5 per cent for the most common childhood cancer.

October 25, 2024
Meet the drivers of clinical trials at SickKids
At the Garron Family Cancer Centre, Clinical Research Associates support innovative clinical trials seeking to improve care and outcomes for children with cancer.

September 24, 2024
"Why does my child have cancer?": Inside the world of cancer genetic counselling at SickKids
As a genetic counsellor in SickKids’ Cancer Genetics Program, Bailey Gallinger helps families who may be affected by a cancer predisposition syndrome.