New discovery finds potential non-antibiotic treatment for cancer-causing bacteria
Summary:
H. pylori is high on the WHO's list of antibiotic-resistant bacteria that pose the greatest threats to human health. This research has shown that harnessing the cell’s own ability to eliminate bacteria inside of stomach cells could be a potential new treatment for H. pylori infection.
Treatment harnesses the cell’s own ability to eliminate bacteria, avoiding the negative effects of antibiotics
Helicobacter pylori (H. pylori) is a type of bacteria that infects the stomach of 50 per cent of people around the world. Despite being exposed to the bacteria, some people will never experience any symptoms and will never need any treatment. However, for those who become infected and, if left untreated, H. pylori can lead to peptic ulcers in the stomach and gastric cancer. Currently, there is no effective vaccine against H. pylori.
H. pylori is difficult to treat, requiring a combination of two to three antibiotics plus a medication to block the production of stomach acid. Even with this complex treatment, it is becoming more difficult to get rid of the bacteria because of increasing antibiotic resistance. The World Health Organization (WHO) has placed H. pylori on its high-priority list of antibiotic-resistant bacteria that pose the greatest threat to human health; urging that new treatments are needed.
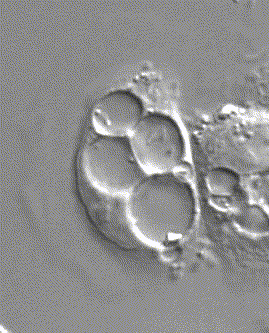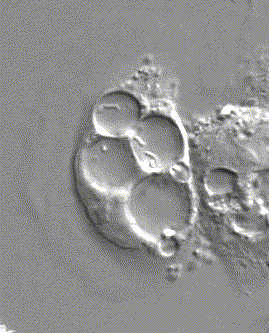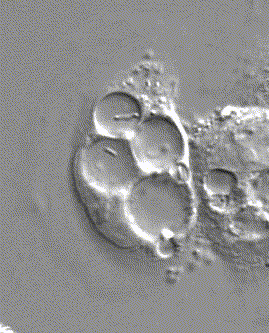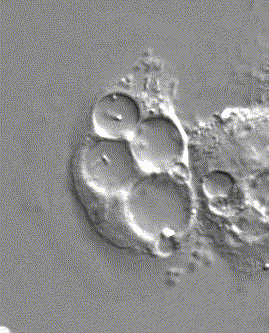
H. pylori swimming in the protected compartment in stomach cells, as seen through a microscope.
This led Dr. Nicola Jones, Staff Gastroenterologist, Division of Gastroenterology, Hepatology and Nutrition and Senior Scientist, Cell Biology, Dr. Mariana Capurro, Research Associate and Dr. Laura Greenfield, Post-doctoral Fellow of The Hospital for Sick Children (SickKids) and their team, to explore a non-antibiotic treatment for H. pylori. Their results were published on May 20, 2019 in Nature Microbiology.
H. pylori secretes a toxin called VacA that enhances the ability of the bacteria to take over the stomach. The team was the first to discover that this toxin allows the bacteria to survive inside of stomach cells in a special compartment. This compartment, called the lysosome, normally kills invading bacteria, like H. pylori. However, the VacA toxin disarms the lysosome of its bacteria-killing ability, allowing H. pylori to survive and hide from antibiotics.
There is a specific channel in lysosomes, called TRPML1, and when activated in infected cells, it restores the bacteria-killing ability of the lysosome, leading to the elimination of the H. pylori. This is the first evidence that TRPML1 could serve as a novel targeted therapy for H. pylori infection.
“Our research shows that we can harness the cell’s own ability to eliminate bacteria,” says Jones, principal investigator of the study and Professor, Department of Paediatrics and Physiology at the University of Toronto. “We were very excited to find a promising new treatment for H. pylori infection that is not an antibiotic and therefore avoids antibiotic resistance and any side-effects of antibiotics.”
These favourable results could lead to future treatment in children and adults suffering from H. pylori infections. The researchers hope to conduct more research before eventually moving to clinical trials.
This work was funded by Canadian Institutes of Health Research (CIHR), Canadian Association of Gastroenterology, North American Society for Paediatric Gastroenterology, Hepatology and Nutrition Foundation, and SickKids Foundation. This is an example of how SickKids is making Ontario healthier, wealthier and smarter (www.healthierwealthiersmarter.com).
